Culture Shift

The human immune system is, in one sense, a detection mechanism. It has evolved, over millions of years, to scan the body for molecular signals that tell it whether to attack or stand down. Most of these signals come from pathogens, damaged cells, or the body’s own hormones. But in 2019, a lab in Germany published a finding that pointed to a much stranger source: one of the signals sensed by the immune system is found in sauerkraut.
When people eat sauerkraut, a molecule called phenyllactic acid (D-PLA) — found in fermented foods — enters their bloodstream and activates a receptor, known as HCA3, on immune cells, triggering an anti-inflammatory response. In addition to lactic acid, phenyllactic acid is one of many compounds produced by lactic acid bacteria during the fermentation of sauerkraut and related fermented foods. Prior to this study, other molecules had been found to bind HCA3, but D-PLA was a hundredfold more potent than any of them.
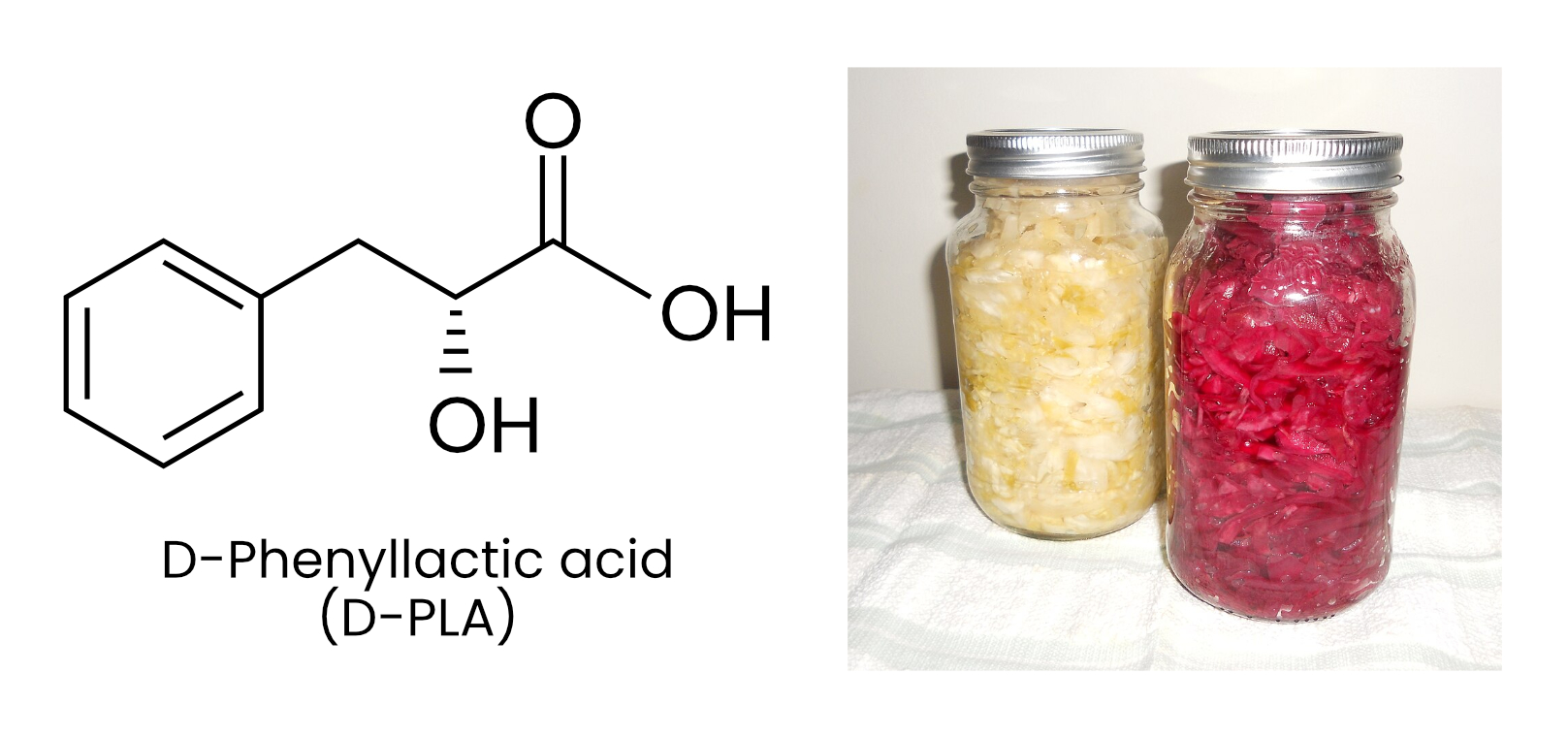
This discovery advances our understanding of how fermented foods can reduce inflammation and positively affect human health. But more striking is what it suggests about hominid physiology. Although HCA3 is part of a larger family of receptors broadly conserved across eukaryotes, HCA3 is only present in humans and other great apes like chimpanzees and gorillas — and not even in other mammals. It is a recent addition to the genome, appearing only a few million years ago. Its existence seems to suggest that our immune system evolved to recognize the microbial metabolites from fermented foods.
We tend to think of fermented foods as something humans invented and then chose to eat. But, increasingly, scientific evidence suggests the causality runs the other way. Fermented foods appear to have helped shape human biology itself, and our bodies may have been built, in part, to expect them. The case for this runs from changes in hominid gut anatomy millions of years ago to the HCA3 receptor, to a growing body of research linking fermented food consumption to immune function and gut health. And it raises an uncomfortable question about what happened when the Western food system, in the name of safety and efficiency, quietly removed these foods from our diets in the nineteenth and twentieth centuries.
{{signup}}
Early Fermentation
Fermented foods are the result of the controlled growth of communities of microbes. At their core, they are the products of the interaction of these microbes and whatever food they consume, whether cabbage or cucumber. While this process varies from food to food, fermentation typically involves managing environmental variables such as oxygen, temperature, and salinity. In contrast to food preservation methods like canning or even pickling, which are designed to prevent microbial growth, fermentation harnesses the capacity of naturally occurring microbes found on fresh food or in the environment to outcompete spoilage organisms.
Most archaeological evidence from pottery shards suggests that fermented food production is at least 7,000 to 10,000 years old. This timeframe coincides with the major transition to agrarian lifestyles, which would have reliably produced surpluses of food and the subsequent need for preservation methods.1 While this explanation satisfies most scholars, there is reason to believe that fermentation may be far older.
For one, it’s a very simple process to trigger. Some foods even ferment spontaneously. In the case of alcoholic drinks, like beer, wine, or mead, ubiquitous yeast species, which are naturally found on grapes and other fruit skins, rapidly use sugar as a food source for reproduction, producing ethanol as a byproduct. The same results occur when ripe fruit falls to the ground and its sugar is exposed to the environment, or when honey is diluted with water.
Other processes require only minimal intervention. For example, submerging fresh food in liquid or burying it creates a low-oxygen environment that encourages the growth of acid-producing bacteria that preserve the food by what is called “lactic acid fermentation.” This technique produces dill pickles, sauerkraut, and kimchi. While salt is often added as an additional intervention against unwanted microbes, it’s not required as it isn’t the primary driver of the fermentation.
Another argument for an earlier origin for fermented foods is that they are found across nearly all human cultures. While the number of fermented foods in the modern, Western diet is fairly limited (cheese, yogurt, bread, chocolate, coffee, beer, wine, kimchi, and kombucha) hundreds more are eaten around the world, from fermented shark in Greenland to a seemingly limitless variety of fermented soy beans in Asia. This diversity is a testament to how humans gradually mastered this ancient practice and modified it to suit new environments as they moved out of Africa.
Around 14 million years ago, our hominid ancestors were arboreal species whose diet would have been primarily based on fresh fruits picked from the trees they lived in. When ripe fruit fell to the ground and underwent spontaneous fermentation, it would have been toxic to our ancient ancestors due to its high concentration of ethanol. Their bodies as yet had no efficient way to break down ethanol.
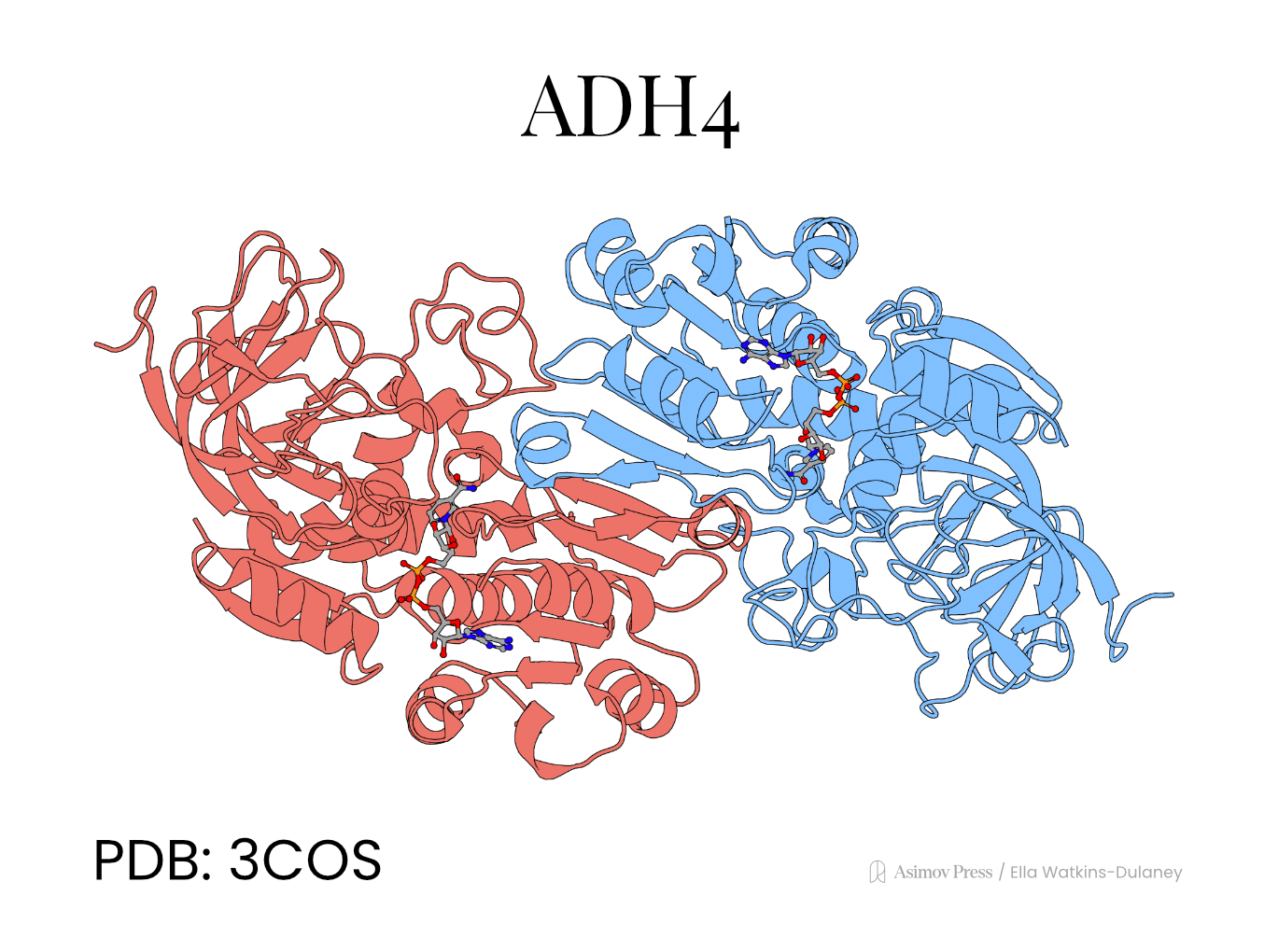
But then, about 10 million years ago, a mutation arose in the genome of the common ancestor of humans, gorillas, and chimpanzees. This mutation, a single amino acid change in the enzyme Alcohol Dehydrogenase 4 (ADH4), enabled it to break down and detoxify ethanol with 40x higher efficiency. The capacity to consume this energy-rich but previously dangerous fruit may even have driven our transition from an arboreal lifestyle to a terrestrial one. What’s more, this ability to tolerate ethanol may have been what allowed our ancestors to diversify their diet and survive while lineages without this mutation went extinct.
The fossil record shows that a major shift in hominid anatomy occurred around 2 million years ago, when hominids developed a smaller rib cage and larger skull. At the same time, another major change took place in their intestines. Compared to our closest relatives, humans have a digestive tract that is 40 percent shorter. This decrease was thought to be driven by the external processing of our food, which reduced the time and energy involved in chewing and digesting. Anthropologist Richard Wrangham argues that the technological innovations of controlling fire and cooking food led to this major change, and that the excess energy we got from cooked food, in turn, supported the evolution of a larger brain.
However, two recent studies, by biological anthropologist Katie Amato in 2021 and evolutionary biologist Erin Hecht in 2023, suggest that these anatomical changes may have been driven by human use of fermentation even before humans began to cook. By allowing microbial species to ferment and break down complex carbohydrates and other macromolecules in foods, we may have turned over certain parts of an otherwise energy-intensive digestive process to microbes in a form of “external digestion.” This use of fermentation to pre-digest food, intentional or not, may have served as a predecessor to cooking, providing the extra calories needed to support the evolution of a larger brain.
Another benefit of fermentation is that it offered access to foods which, previously, would have been toxic. As our ancestors came down from the trees and needed new ways to fill their stomachs, the tubers of many plants and grasses offered an appealing, ready source of calories. Tubers contain large deposits of starch. Root vegetables, such as potatoes, yams, and carrots, are our modern-day, highly domesticated equivalents. But the wild tubers of our ancestors’ time were hard to chew, and some contained low levels of toxins. Varieties of cassava, for example, contain compounds that release cyanide when ingested. After just a few days of fermentation, however, microbes destroy these dangerous molecules and make the food safe to eat.2

Ultimately, given the simplicity of the fermentation process, its provision of new food sources, and its role in decreasing the need for extensive chewing and digestion, fermentation could have had an outsized impact on human evolution. It may, in fact, have helped make us human.
Peril and Promise
Perhaps the most striking thing about fermentation is that humans figured out how to control the growth of microbial species long before we understood what “microbes” were.
No one had seen microbial life until the 17th century, when Dutch scientist Antonie Van Leeuwenhoek used a handmade microscope to reveal small, motile forms he described as “animalcules.” It wasn’t until the late 1800s, however, that the French chemist Louis Pasteur demonstrated the role of microbes through his studies of fermented foods. His work on the spoilage of beer and wine formed the basis of the “germ theory” of disease. If microbes could be the causative agents of spoilage in food, Pasteur reasoned, maybe they could also be the causative agents of disease.
For his part, Pasteur was not strictly “anti-microbe.” He found them enthralling, investigating the differences between lactic fermentation (yogurt, pickles, and sauerkraut), butyric fermentation (butter, cheese, and milk), and acetic fermentation (kombucha, sourdough, sour beer), as well as developing the categories “aerobic” and “anaerobic” (which refer to whether microbes require oxygen to survive).
Even so, Pasteur’s work identifying microbes responsible for putrescence and disease has had the greatest impact on our food system. At the beginning of the twentieth century, automated machinery expanded canning capacity from roughly 10 cans a day to 1,000. Variation in the quality of the sealed lids, temperature treatments, and exposure to contaminants through handling meant a greater potential for microbial illnesses like botulism.
After three deadly botulism outbreaks in 1919 linked to California-distributed olives, the canning industry turned to Pasteur-inspired “bacteriologists” to design better canning systems and restore public confidence. While the resulting practices — including steam sterilization, the marking of batches, and traceable can coding — were at first voluntary, the Cannery Act of 1925 mandated statewide compliance.

By the mid-1900s, microbial research into food had come to focus on how to keep organisms out of it. Innovations in heat, pressure, refrigeration and anti-microbial agents to extend shelf life and decrease potential contamination with food-borne pathogens formed the core of academic and industrial research. As our methods of food production shifted, so did our diets. Americans largely moved away from the consumption of traditionally fermented foods, with one major exception.
That exception began with a single lecture. The Russian zoologist, Ilya Mechnikoff, based at the Pasteur Institute in Paris, was well known in the early 1900s for his scientific discoveries involving the immune system, for which he would win the Nobel Prize. But towards the end of his career, Metchnikoff became fascinated with the idea that aging was just another disease awaiting a cure.
In his 1908 book, The Prolongation of Life, Metchnikoff proposed that this disease was caused by "putrefying" microbes that lived within the human gut, or, as he put it, “chronic poisoning from an abundant intestinal flora.” His suggested cure came in an unexpected form — yogurt. Mechnikoff reasoned that just as the acid in sour milk prevented the growth of spoilage organisms, it might limit the growth of “spoilage” microbes in the gut.
After speaking with a student after one lecture, Metchnikoff learned of large numbers of centenarians in Bulgaria (one of whom he credulously reported as being “158” years of age).3 Metchnikoff hypothesized that the consumption of large quantities of yogurt in Bulgaria prevented aging through the action of lactic acid on gut bacteria. After obtaining a sample of the “Bulgarian bacillus” (Lactobacillus delbrückii subsp. bulgaricus) from yogurt, he set out to study the effects on the gut. His lab work showed that the presence of the yogurt microbe and the lactic acid it produced slowed the growth of intestinal microbes.

Metchnikoff thus advised the consumption of yogurt to promote healthy intestinal balance, writing: “A reader who has little knowledge of such matters may be surprised by my recommendation to absorb large quantities of microbes, as the general belief is that microbes are all harmful. This belief, however, is erroneous. There are many useful microbes, amongst which the lactic bacilli have an honourable place.”
Metchnikoff initially presented his yogurt hypothesis at a public lecture in 1904 in Paris, titled “Old Age.” The lecture went the early 1900s equivalent of viral. Newspapers ran stories with headlines like “Drink Sour Milk and Live to be 180 Years Old” (Evansville Courier and Press) and “Sour Milk is Elixir: Secret of Long Life is Discovered by Prof. Metchnikoff” (Chicago Daily Tribune). “Within months of Metchnikoff’s lecture, milk-souring germs had blossomed into an international business. Pharmacies throughout Europe and the United States were offering Bulgarian cultures in the form of tablets, powders, and bouillons — to be consumed as is or used,” writes Luba Vikhanski in her book Immunity. It was, in effect, the first “superfood.”4

“Probiotic” products quickly followed, containing dehydrated “lactic bacilli,” that anyone could use to sour their own milk in the way prescribed by Metchnikoff. But despite interest in yogurt and probiotics as health foods, most 20th century microbiologists remained focused on “bad actors,” the microbes and pathogens involved in disease. However, this changed toward the end of the century with advances in sequencing technology and chemical analysis techniques like mass spectrometry, which allowed them to probe microbial genetics and metabolism more closely and with more nuance.5
Environmental DNA sequencing revealed the diversity of microbial species across habitats, including in and on the human body as well as in our food. Understanding what these microbes are doing, and how, has become one of the challenges of modern microbiology.
To Eat Microbes
In response to this challenge, a lab at Stanford University, led by Erica and Justin Sonnenburg, has been doing seminal work on the human gut microbiome and how species within it function and interact. Recently, the Sonnenburgs have turned their focus on diet-microbiome interactions to fermented foods. A clinical trial, which the Sonnenburgs set up in collaboration with nutrition scientist Christopher Gardner in 2021, offered the clearest evidence to date that fermented foods are essential for gut health. In the trial, 36 healthy adults spent 10 weeks eating a diet high in such foods.
At the end of the study, they showed increases in gut microbiome diversity, which is generally associated with gut health. (The participants had new microbial species in their guts, which did not come from the fermented foods. It seems, rather, that fermented foods somehow make the existing gut ecosystem more receptive to incorporating new strains.) Perhaps an even more impactful outcome was that the researchers also found widespread decreases in inflammatory markers in the blood of these participants.
Given that low levels of inflammation sustained over time, referred to as chronic inflammation, is believed to be implicated in many diseases, the ability to decrease it though simple dietary changes would be welcome. However, the six servings of fermented foods a day consumed by the study participants is far higher than that in most U.S. diets. While yogurt and cheese are commonplace, with an average of 13.8lbs and 42.3lbs consumed per person per year respectively, this represents about a serving of fermented dairy a day. Fermented vegetables also comprise less than a serving per day. The impressive 387 million pounds of sauerkraut Americans consume per year equates to only 1.5lb per person, or about 0.06 servings a day.6 There has been a resurgence in interest in fermented foods, from high-end chefs experimenting with new types of fermentations to home fermenters caught up in the pandemic sourdough craze, but we have a long way to go before consumption reaches levels needed for clinically meaningful outcomes.
Even larger gaps remain in our understanding of how fermented foods actually drive health benefits. Beyond inflammation, fermented food consumption has been associated with a wide range of positive health outcomes, from gut health to mental health. As compelling as the Sonnenburg study is, it doesn’t yet reveal the mechanism(s) by which fermented foods trigger changes in human physiology.
While the 2019 sauerkraut study points to the importance of microbial metabolites like phenyllactic acid, if we co-evolved with fermented foods over millions of years, this example of a metabolite-receptor pairing is likely just the tip of the iceberg. As in many other areas of microbiome research, we need to move beyond correlation to causation. Doing so will require a much deeper understanding of the molecular composition of fermented foods, how they are connected to human biology, and more precise clinical studies.
Scientists are beginning to recognize the potential diversity of bioactive metabolites in fermented foods, but most studies focus on a single food type at a time and use different assays of bioactivity from lab to lab. To be able to effectively map the complex interactions between fermented food microbes, metabolites, and human biology, we need larger, consolidated datasets.
To this end, the Microcosm Foods project has been assembling a first of its kind collection of fermented food data pairing metagenomics (mapping microbes), metabolomics (mapping metabolites), and transcriptomics (mapping changes in human immune cells upon exposure to fermented foods) across over 100 different foods. Open-source, systematically-acquired datasets such as these will help build the scientific foundation needed to untangle these complex interactions.
For most of human history, people harnessed microbial ecosystems to make fermented foods and reaped the benefits without understanding their mechanism. Then, in a period of roughly 100 years, the Western food system replaced them with sterile, shelf-stable alternatives.
Today, we are finally beginning to understand how fermented foods interact with our biology — through receptors like HCA3, through shifts in gut microbial diversity, and through inflammation pathways. Science is catching up to what fermentation has been doing all along.
{{divider}}
Rachel Dutton is a microbiologist studying fermented foods, from their use as microbiome models to their impacts on health. She received a PhD in Microbiology and Molecular Genetics from Harvard University, and led academic labs at Harvard and UC San Diego. Rachel is currently a Resident at the Astera Institute and a Fellow in the Big If True Science program at Renaissance Philanthropy.
Credit: Header by Ella Watkins-Dulaney. L. reuteri image by Anastasiia Dmytriv.
Cite: Dutton, R. “Culture Shift.” Asimov Press (2026). DOI: 10.62211/92yr-34qw
Footnotes
- Preservation isn’t the only benefit of fermentation, however. It also completely transforms raw ingredients, adding new flavors, textures, and aromas. These changes are dictated by microbial metabolism, which produces not just primary products of fermentation like acids, but also a diverse collection of enzymes and flavor molecules.
- Cassava is the third most important dietary staple around the world after rice and corn. The fermented starch that comes from this quick-ferment is used as the starting point for many different staple foods such as fufu in Nigeria or pao de quiejo, also known as Brazilian cheese bread.
- In his essay on Metchnikoff, blogger H.D. Miller writes “Unfortunately, reports of Bulgarian longevity seem to have been greatly exaggerated. Indeed, the best current guess is that Bulgarian life expectancy at the turn of the last century was actually only 40.08 years, more than a few decades short of a century. As with Sardinians and Okinawans more recently, Bulgarians were better at convincing outsiders they were very old than actually being very old.”
- This is an amazing lecture on the history of yogurt.
- Today, we know that many, if not most, species of microbes on the planet do not grow well under standard lab conditions, which limits the usefulness of earlier culturing methods.
- A single serving size for yogurt is 170g (or ¾ cup), cheese is 42g (about a 1 inch cube), and sauerkraut is 30g (2 tablespoons). Based on the reported average annual per person consumption in the US, the average daily consumption is 0.1 servings of yogurt, 1 serving of cheese, and 0.06 servings of sauerkraut.
Always free. No ads. Richly storied.
Always free. No ads. Richly storied.
Always free. No ads. Richly storied.